Medical ‘Miracles on 34th Street’ at Penn Medicine
Below are abbreviated stories from Penn Medicine News. View full stories at https://www.pennmedicine.org/news
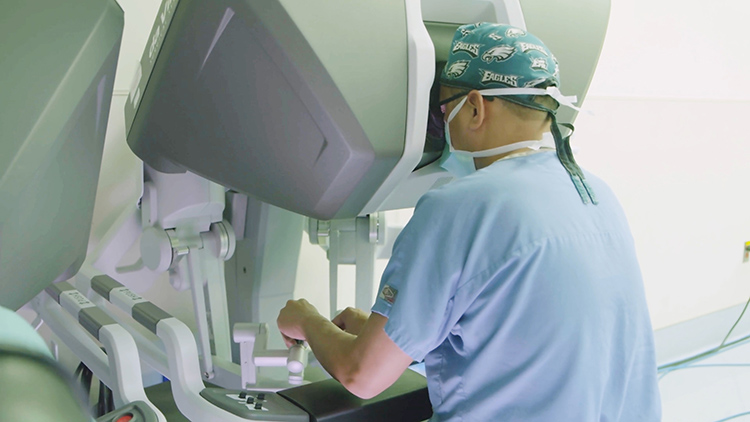
First Robotic Bilateral Breast Reconstruction
A team of surgeons from Penn’s Perelman School of Medicine are the first in the world to use a surgical robot to assist with a bilateral free flap breast reconstruction—a procedure in which tissue is taken from the lower abdomen (similar to a “tummy tuck”)—and used to rebuild the breast. The robot enables surgeons to make a much smaller incision into the abdominal wall muscles, allowing patients to recover and be discharged more quickly and without the use of addictive narcotic painkillers. Suhail Kanchwala, an associate professor of plastic surgery, led the team that performed the procedure, which took place at Pennsylvania Hospital in December. Dr. Kanchwala partnered with Ian Soriano, a clinical assistant professor of surgery who specializes in minimally invasive procedures, to develop the technique.
“We’ve been using a minimally-invasive, laparoscopic technique to reduce pain and get patients home more quickly without using narcotics for more than a year. The addition of the surgical robot allows for greater precision and is the next step in our evolution,” Dr. Kanchwala said.
Women who have chosen a mastectomy, either to remove cancerous breast tissue or as preventative measure due to genetic risk, have several options for reconstruction. Traditionally, using a patients’ own tissue results in a more natural appearance and is a more permanent solution when compared to implant-based reconstructions, which often require additional surgeries. Penn surgeons perform more than 700 tissue-based reconstructions yearly, making it the largest center for this form of reconstruction in the world.
“Our experience is what allows us to innovate, and adapting minimally invasive approaches to breast reconstruction allows patients to have the same recovery of implant reconstruction without the downsides of having an implant, such as the risk of infection or the need for further surgery,” Dr. Kanchwala said.
The minimally invasive flap procedure virtually eliminates the need to cut into a patient’s abdominal muscles to remove the skin and fat of the lower abdomen to use in the reconstruction of the breast. That incision in the muscle is the main source of pain and other potential complications. Dr. Kanchwala called the laparoscopic technique, which he has now used in more than 120 cases, “game changing.” He also noted that in 70 percent of those cases, his patients did not require any narcotics, even while under anesthesia. Instead, patients received over-the-counter medicine like Motrin or Tylenol for pain.
“Many of these patients wake up as if they haven’t had a surgery, and we’ve seen patients who would normally be in the hospital for five days go home in just one or two days,” Dr. Kanchwala said.
Much like with the laparoscopic technique, the surgical robot allows the surgeon to avoid larger cuts to the muscle while also collecting blood vessels more easily. The smaller incision also limits the risk of hernia and other complications.
Pain management is another unique aspect of this technique. Research has shown that one out of every 20 breast reconstruction patients who have never had a narcotic before their surgeries are still on those narcotics five years later. Dr. Kanchwala said this technique addresses this reality head-on, and it requires a team approach. All patients are enrolled in a coordinated Enhanced Recovery Protocol, which means from the minute they enter the hospital the focus is on their recovery and getting them back to normal as fast as possible.
“We’ve paired our surgical innovations with similar progressive ideas in anesthesia and postoperative care,” Dr. Kanchwala said. “Nothing I do now is the same as it was even a year ago, and knowing what I now know, I could never go back.”
Gaining Strength in Treatment of Spinal Muscular Atrophy
Lauren Elman, an associate professor of neurology, has spent part of her career caring for a group of patients with no treatment options. The genetic disease, spinal muscular atrophy (SMA), can strike beginning at birth and robs patients of their ability to walk, eat and breathe. SMA is the leading genetic cause of death for infants and the second most common autosomal recessive disease—a disease inherited through two mutated genes—occurring in about 1 in 10,000 people. But now, there’s hope in a new treatment option.
The United States Food and Drug Administration announced the approval for Spinraza (nusinersen) in December 2016, making it the first-ever FDA-approved therapy for SMA. The clinical trials for the drug showed improved motor function in young patients with the most severe forms of SMA. While there is only limited data on the effectiveness of the drug in adults, the FDA approved its use for all patients who are confirmed to have the gene mutation which causes SMA.
That approval started Dr. Elman on her quest to bring the therapy to patients at Penn Medicine.
“As soon as the FDA approved this therapy, our patients were asking for it,” explained Dr. Elman. “It took hard work to create an SMA treatment program here for adults, but I’m proud to say that we’ve been up and running since August 2017. We were the first center in Philadelphia to offer treatment to adults and we’re the largest program in the area.”
There are four types of SMA, characterized by the severity of disease symptoms. SMA type 1 is the most common and occurs within the first six months of life. Babies typically have difficulty breathing, sucking and swallowing. Children with type 1 are unable to sit without support and most only live a few years due to complications with breathing. SMA type 2 has onset between the age of 7 months and 18 months. Children with SMA type 2 may reach motor milestones such as sitting independently, but few are able to stand or walk unaided. SMA type 3 occurs in older children and teens who learn to stand and walk, but lose the ability later in life. SMA type 4 affects full-grown adults, with onset typically in the second or third decade of life.
Thanks to the new therapy, some children are learning to stand and many are sitting unassisted—abilities unheard of before treatment. Many others may not experience any further loss or deterioration of skills. For adults, the effect of the drug is less clear with possibilities including improvement in or stabilization of symptoms, with the hope that no additional function will be lost.
“When I learned about SMA in medical school it was untreatable. We were just starting to learn what caused it. Now, there’s a treatment that’s truly remarkable,” Dr. Elman said. “Stopping progression in a neurodegenerative disease is a home run. And any improvement—that’s a grand slam. I have some patients who’ve had reflexes return that were gone for years. This just has not happened before in diseases like this. It’s truly astonishing.”
The treatment—which is administered through an injection into the spinal fluid—can be difficult as many patients have complicated anatomy resulting from scoliosis (a curvature of the spine common in SMA patients). Interventional radiology experts ensure the treatment is delivered to the right location. There is also a complicated dosing schedule—four doses are given over a 10-week loading period, with a maintenance dose given every four months thereafter. By developing a multidisciplinary effort between teams in neurology, radiology and pharmacy, patients are now able to get the treatment they need.
There are research initiatives and clinical trials underway, bringing more hope for future breakthroughs. Dr. Elman says gene therapy for SMA could be possible since the disease is caused by the deletion or mutation of a single gene, and because a good vector for delivering a replacement gene is available. The vector being used to study gene replacement therapy for patients with SMA is the adeno-associated virus (AVV), which is a vector that has already been successfully used in people.
“Patients have hope where they never had hope before,” Dr. Elman said. “It’s the most rewarding thing I have ever been part of.”

First Robot-Assisted Spinal Surgery
Noah Pernikoff is back to his life in New York City after becoming the first patient in the world to undergo a complex three-part, robotic-assisted surgery. The robotic arms made it possible for the multidisciplinary team at Penn to successfully remove a rare tumor from his neck, where the skull meets the spine. The groundbreaking surgery was completed by a multi-surgeon team, led by Neil Malhotra, associate professor of neurosurgery, at the Hospital of the University of Pennsylvania in August 2017 over a span of two days and more than 20 hours.
Chordoma is a rare type of cancer that occurs in the bones of the skull base and spine. A chordoma tumor usually grows slowly and is often asymptomatic for years. In the case of 27-year-old Mr. Pernikoff, a 2016 car accident revealed his surprising diagnosis.
Among his injuries from the accident, Mr. Pernikoff—who was working in New York City for a commercial contracting firm—tore his rotator cuff and had several herniated discs. More important, however, was his post-accident nagging neck pain, which led to an x-ray that revealed a concerning lesion in his neck, on his cervical spine. The lesion was clearly unrelated to the accident, and far more concerning than the minor injuries he had endured. After making a recovery from the accident, Mr. Pernikoff’s father, a physician, encouraged his son to see a neurosurgeon for evaluation of the injury. The neurosurgeon Mr. Pernikoff saw ultimately recommended a biopsy of the spot, which resulted in a diagnosis of chordoma.
“I’m lucky because they caught mine early. For a lot of people, if it’s not found and treated early, it’s lethal,” Mr. Pernikoff said. “The doctor said if I hadn’t discovered it through the car accident it probably would have kept growing until it came to a point on my spinal cord where it caused paralysis or death. I feel very lucky in that regard.” Unfortunately, the neurosurgeon explained to Mr. Pernikoff, while surgery is known to be the best option for chordoma, Mr. Pernikoff’s would be too difficult to resect and he would have to try the second option, radiation with proton therapy.
Chordoma is extremely rare; it affects only one in 1 million people each year. Mr. Pernikoff’s specific type of chordoma, located on his C2 vertebrae, is even rarer, making treatment a challenge. Mr. Pernikoff’s neurosurgeon immediately referred him to Penn, where a multidisciplinary team reviewed his case, and his options, and began crafting a treatment plan—not through radiation, but a complex surgery that had never been performed before.
Neil Malhotra, an assistant professor of neurosurgery and orthopaedic surgery and the vice chair of operations in the department of neurosurgery, gathered a multidisciplinary team of physicians to treat Mr. Pernikoff’s chordoma. Dr. Malhotra planned to remove the tumor through a rare and complex spinal surgery approach. Bert W. O’Malley, Jr., professor and chairman of the department of otorhinolaryngology: head and neck surgery, planned to aid Dr. Malhotra and improve Mr. Pernikoff’s recovery by using a trans-oral robotic (TORS) approach for the second part of the surgery. TORS is the world’s first group of minimally invasive robotic surgery techniques, invented at Penn, to remove benign and malignant tumors of the mouth and throat.
“This would be a first-ever use of a robot in this manner—a rare approach to an already rare and complex case,” Dr. Malhotra said. “Our team needed to reconstruct the removed area of Mr. Pernikoff’s spine using bone and rods, and that was only the beginning.”
The stakes were high. Because of the placement of the tumor, Dr. Malhotra said removal could compromise the structural integrity of Mr. Pernikoff’s spine, causing permanent paralysis. There was also a risk of complications such as bone and tissue breakdown, loss of sense of smell and fine motor skill issues. And, he added, “if we couldn’t remove the entire tumor, it would likely grow back, perhaps more aggressive than before.”
The surgery was performed in three parts. First, the neurosurgeons went through the back of Mr. Pernikoff’s neck and cut the spine around the tumor to prepare for the second stage, removing the tumor through his mouth. The key to this stage would be to make ultrasonic bone cuts—removing a piece of bone—around the tumor without touching it, and without injuring the spinal cord that lay between the neurosurgeon and the tumor/spinal column. With stage one success, Dr. O’Malley and a team of three head and neck surgeons used the surgical robot to clear a path so Dr. Malhotra could remove the tumor, and part of the spinal column, in its entirety through the mouth. Finally, the team reconstructed Mr. Pernikoff’s spinal column, which was now missing an important bone in his neck, using some of Mr. Pernikoffs’ own bone from his hip and rods to finalize stabilization of the newly built portion of his spine.
“The capability of this technology and procedure is revolutionary,” Dr. O’Malley said. “This surgery was groundbreaking and it’s a wonderful example of how versatile TORS is for tumors in the head, neck, and now spine.”
Nine months after surgery, Mr. Pernikoff was back to work and said he’s forever grateful for the car accident that revealed his diagnosis and the life-saving care that he received at Penn Medicine.
Medical Miracles at Penn Veterinary Medicine
Below are abbreviated stories from Penn Vet Extra. View full stories at www.vet.upenn.edu/about/press-room/publications/penn-vet-extra

Cat-tastrophe
At only two months old, Bridget the kitten has had a lot of close calls. She was thrown from a stranger’s car off the South Street bridge in Philadelphia—where she landed, miraculously unharmed—and was rescued and fostered by Ariel Smith, who named her after the ordeal. After a few weeks in the safety of Ms. Smith’s apartment, though, Bridget ran headfirst into yet another death-defying situation.
“She and my two cats had become buddies by then, and liked to chase each other at breakneck speeds back and forth across the room,” said Ms. Smith. “They came bolting by and I heard a crash, then looked over and saw a gaping window. My heart just stopped. It was a horrifying moment.”
Bridget had somehow managed to dislodge the open window’s screen, tumbling four stories to the pavement below. Ms. Smith and her partner frantically searched for her and eventually found her panting underneath a parked car, bleeding from her mouth. “We knew we had to get her checked out, and that every second counted,” Ms. Smith said.
She rushed her kitten to Ryan Hospital’s emergency service, where veterinarians stabilized her and searched for broken bones before admitting her to the Intensive Care Unit overnight.
“Bridget suffered from classic ‘high rise disorder’,” said Lori Waddell, clinical professor of emergency and critical care, who monitored Bridget in the ICU. “We see this a lot in the warmer months. Cats fall off of balconies or windowsills, and have a range of injuries to their upper bodies. They come in with cranial and oral fractures, internal bleeding, abrasions, broken ribs, that sort of thing.”
X-rays taken at Ryan Hospital showed that several of Bridget’s ribs were indeed broken. Tiny tears in her lungs had also caused air to leak into her chest cavity, making it difficult for her to breathe. The hospital immediately removed the trapped air with a needle, freeing up space for her lungs to expand, put her on fluids and pain medication and placed her in an oxygen cage to help slow her rapid breathing. After three days of monitoring, she was eventually released back to Ms. Smith’s care.
“That’s pretty amazing given the amount of trauma she could have had,” said Dr. Waddell. “Other cats aren’t as lucky. It’s really important for owners to secure windows and keep cats away from terraces or balconies where we could see them fall. They’re amazingly curious animals, so if they see a bug or bird going by, they’ll jump for it. In a city environment, that can be really dangerous.”
Bridget made a full recovery, and was back to chasing her foster brothers around Ms. Smith’s apartment. “At less than a year old, she’s already been through a lot, but she has an unbreakable spirit. She’s a sweet girl with energy and love to spare,” said Ms. Smith.
Despite her rough beginnings, Bridget’s story has a happy ending. In early September, Ms. Smith and her partner found a “forever” home for Bridget—with a loving family that plans to keep their windows securely closed.

Surprise! It’s Twins!
Excitement over a first pregnancy turned to concern for owner Adel Dukes Melson when her pregnant Holsteiner, Treasure, began showing signs of premature foaling. Weeks before the mare’s March 13 due date, her mammary gland started to develop and secrete milk, a typical indication that her body was preparing to soon give birth.
On February 19, Ms. Melson and Treasure traveled two hours from their home in Bethany Beach, Delaware, to Kennett Square, Pennsylvania arriving at New Bolton Center’s Emergency & Critical Care department at 8:30 p.m.
There, they met Michelle Linton, staff veterinarian, neonatal intensive care specialist and part of Penn Vet’s High Risk and Healthy Mare Foaling programs. That night, Dr. Linton and her team performed a physical exam, transrectal ultrasound and fetal heart rate test. The next morning Treasure received an abdominal ultrasound to assess the fetus, uterus and placenta.
Dr. Linton was expecting to find placentitis, the most common reason for premature mammary gland development and a potentially life-threatening condition for mare and foals.
“Treasure came in as a likely placentitis case, and we treated her as one,” Dr. Linton said. “But her uteroplacental measurements were normal, suggesting we were maybe dealing with something more.”
Although the ultrasounds showed one fetus and one heartbeat, Dr. Linton suspected Treasure might be carrying twins, which could also explain early udder development—and which, surprisingly, can be easy to miss in prenatal exams. She admitted the mare—317 days pregnant at this point—to the Neonatal Intensive Care Unit for monitoring and rest. Over the next few weeks, Treasure grew bigger and bigger but didn’t go into labor.
Finally, on March 13, Dr. Linton’s suspicions were confirmed. At 338 days of gestation, Treasure began foaling. At 9 a.m, the mare gave birth. Not once, but twice.
“As soon as I saw the legs, it was obvious the foal—a filly—was very small,” Dr. Linton recalled. “And pretty much straight away this first set of legs was followed by a second set of legs belonging to a colt.”
Treasure successfully delivered twins—Ms. Melson named the filly Cherish and the colt Cache.
“Twins can be hard to diagnose during late gestation,” explained Dr. Linton. “The bodies were aligned in utero so we could only visualize one thorax and heartbeat.”
While Dr. Linton triaged care of two foals, Ms. Melson, who had left home as soon as she got the labor call, was just arriving.
“There was a special buzz in the hospital. Dr. Linton came out to meet me with a big grin on her face but waited to tell me anything,” Ms. Melson laughed. “When I got to Treasure, I saw the two amazing little foals. Treasure was absolutely beaming and thrilled with herself. I was shocked.”
Treasure and her duo is a rare case. In horses, twin fetuses are uncommon. Carrying them to term is even more unusual, and birthing healthy twin foals is especially unlikely.
“Twin pregnancies are extremely undesirable in horses, as they almost always have a bad outcome,” said Dr. Regina Turner, associate professor of reproduction and chief of the Reproduction & Behavior Service. “If allowed to progress through gestation, twin pregnancies almost always end in late-term abortion of both foals, or the birth of small, growth-retarded foals that either are born dead or severely compromised.”
Fortunately, this isn’t the situation for Cherish and Cache. Though small at birth—about 49 pounds for Cherish and 47 for Cache—both were born healthy to a mare that Dr. Linton said, “is a great mother and cut out for the job.”
“With twins, our immediate concern is the strength of their lungs and kidneys—are the organs mature enough and functioning properly?” explained Dr. Linton. “We also worry about whether their carpal (knee) and tarsal (hock) bones have ossified completely. The cuboidal bones, which are small bones located in those joints, are the last to make the conversion from cartilage to bone. Incomplete ossification of cuboidal bones can lead to collapse of the joints and degenerative joint disease.”
Cherish’s and Cache’s organs checked out fine. The main problem, explained Dr. Linton, was the foals’ size. “Even though Treasure carried them to term, they had in utero growth restriction. Initial X-rays confirmed incomplete ossification of the carpal and tarsal bones in both foals.”
The foals had to be kept quiet and off their feet to encourage proper bone growth. Strictly confined, they remained with Treasure at New Bolton Center for two months. The three horses were under the careful, round-the-clock watch of the NICU team and foal sitters, volunteers who assist clinicians and staff in caring for mares and foals during the foaling season.
Slowly but surely the twins’ bones ossified, and they increased their activity, such as having supervised nursing sessions with Treasure. They gained weight and got stronger every day. Playful from almost day one, it wasn’t easy to keep the feisty twins calm while they grew.
“They have become so rambunctious, up and down all the time,” said Ms. Melson at the time. “Initially, we had to discourage them from standing, but since they worked out how to stand, the care team has had its hands full!”
In the meantime, Ms. Melson’s shock at having twins has now given way to pure joy and gratitude that Treasure delivered two thriving foals. (Ms. Melson started a Facebook page to share their growth and antics.)
“Treasure and the twins are receiving excellent care from a wonderful team. At every stage, the veterinarians, students and staff have been very hands-on. Everyone cares so much about mom and her foals,” Ms. Melson commented. “New Bolton is very special place.”
Now Cherish, Cashe and Treasure are back home and doing very well.

Physical Rehab Helps “Rock Star” Ranger Walk Again
On a Sunday in August, Cory Laslocky’s son Nathan left for overnight camp. The family’s four-year-old Australian cattle dog Ranger happily bid his human buddy goodbye. The following morning, Ranger was limping. By the end of the day, he was unable to stand and didn’t respond to any touch of his hind limbs.
“I rushed Ranger over [to my vet] as soon as I got home from work,” recalled Mr. Laslocky. “The doctor suspected a neurological issue and recommended we go right to Penn Vet for evaluation. Ranger was admitted immediately that night.”
An MRI found a ruptured spinal disc. Scott Petesch, a resident in neurology and neurosurgery, performed surgery. Even though surgery went smoothly, the dog faced just a 50% chance of regaining use of his back legs, and he would need intense physical therapy. His Penn Vet care team grew to include Molly Flaherty, staff veterinarian in physical rehabilitation medicine, and physical rehabilitation medicine nurse Allison Kyler.
The day after surgery, Dr. Flaherty and Ms. Kyler started Ranger’s inpatient rehab program. “We began with acupuncture to stimulate his nerves and laser therapy to increase cellular energy for healing—both also help with pain relief,” said Dr. Flaherty. “We also did some standing exercises. Because Ranger couldn’t stand or move his legs on his own, we used an inflated peanut ball to support his body weight and mimic the natural sensations of standing.”
After a week, Ranger was discharged with a home-care plan, pain medications and a lineup of Penn Vet visits. Weekly, Mr. Laslocky brings him to Penn Vet for physical therapy: movement activities, acupuncture and laser treatment to facilitate healing, pain relief and mobility. He and his son also take Ranger through prescribed exercises and monitor his activity. Ranger also underwent regular hydrotherapy at an outside facility.
“On his first post-op visit, Ranger could move his back legs a bit, but he wasn’t yet standing or walking,” said Dr. Flaherty. “A week later, he was able to stand on his own and take a few steps before falling. By mid-September, he could take several steps without stumbling. We then increased his activity, adding more involved movements. At the end of September, a month after his surgery, I met Cory and Ranger in the Ryan Hospital lobby, and Ranger proudly walked in on his own.”
Dr. Flaherty acknowledges that owner dedication plays a large role in such cases. “Ranger would not have had this kind of progress if his owners were not so dedicated to him and committed to his rehabilitation work,” said Dr. Flaherty, who joined Penn Vet in May 2018 to help expand Ryan Hospital’s Physical Rehabilitation Medicine Program. Although the program’s services are currently available only to Penn Vet patients with an internal referral, Dr. Flaherty has plans to open it to outside referring veterinarians. She also wants to add new staff and services.
Mr. Laslocky and his son view Ranger’s rehab as a part of their daily routine—and it also helps, said Mr. Laslocky, that they have a deep bench of friends and family to support the pup’s care. Mr. Laslocky has been especially thankful for Penn Vet’s comprehensive approach to Ranger’s treatment and recovery. “Whenever there’s a potential problem or something to check out, neurology experts are in the same building, and Dr. Petesch or Dr. [Greg] Kaiman can check in on Ranger while he’s doing PT.
“Ranger has become a rock star at Penn Vet. When he walks into the hospital, people I don’t know greet him and spread the word that ‘Ranger’s in the house.’”
Penn Buildings Aglow for the Holiday Season
From English Tudor to French Chateau, from Georgian to modern, the one common denominator of these buildings at this time of year is that they are each decked out with twinkling lights outside or inside. These are just a few of the Penn buildings on campus that are aglow for the holiday season.

The Phi Gamma Delta (nicknamed “Phi Gam” or “FIJI”) fraternity house, designed by American architect Walter Mellor in the early English Tudor style, was built at 3619-21 Locust Walk in 1914. He earned a BS in Architecture from Penn in 1904 and was himself a member of Phi Gamma Delta. The Beta chapter, which was established at Penn on March 3, 1881, resided in this building from 1914 until 1999 and then from 2008 until the present day.

Penn’s President’s House, also known as Eisenlohr Hall, so named for the West Philadelphia cigar manufacturer Otto C. Eisenlohr who had the grandly classical mansion designed by Horace Trumbauer at the height of his career. This elegant French chateau is one of the gems of Trumbauer’s career. It was renovated into the University of Pennsylvania’s President’s House in the early 1980s first becoming the official home to the Hackneys and then subsequent Penn Presidents (Almanac December 2, 1980).

The Kappa Sigma (colloquially “Kappa Sig”) fraternity house was designed by architect Theodore Epps and built at 3706 Locust Walk in 1924. The Georgian style building houses the Alpha-Epsilon chapter of Kappa Sigma, which was established at Penn on January 20, 1892. Kappa Sigma currently has 320 active chapters and colonies across North America, making it one of the five largest international fraternities.

The Annenberg School is a good example of 1960s classic modern architecture, altered and extended by Mitchell/Giurgola Architects in the 1980s in a way that acknowledged the character of the original building, but with the richer urban flavor of the architect’s best work. Four audio-visual classrooms were added under the Annenberg Plaza as part of the $9.6 million renovation to the School (Almanac November 12 1985). In 2004, the Annenberg Plaza (above) was dedicated on June 17 with a ribbon-cutting by the Honorable Leonore Annenberg and then Penn President Judith Rodin, as Dean Michael X. Delli Carpini watched. With funding from the Annenberg Foundation, the Plaza received an upgrade including handicap access to the Annenberg Center, new granite paving and landscaping to soften the appearance.
 A research team led by University of Pennsylvania professor of medicine, epidemiology, and medical ethics and health policy, and LDI senior fellow Scott Halpern has received an $11 million grant from the Patient-Centered Outcomes Research Institute (PCORI) to develop the largest study ever done comparing different strategies to help lung cancer screening patients to stop smoking.
A research team led by University of Pennsylvania professor of medicine, epidemiology, and medical ethics and health policy, and LDI senior fellow Scott Halpern has received an $11 million grant from the Patient-Centered Outcomes Research Institute (PCORI) to develop the largest study ever done comparing different strategies to help lung cancer screening patients to stop smoking.
 Virginia Lee, the John H. Ware 3rd Endowed Professor in Alzheimer’s Research at the Perelman School of Medicine at The University of Pennsylania, received the 2018 Robert A. Pritzker Prize for Leadership in Parkinson’s Research from the Michael J. Fox Foundation for Parkinson’s Research (MJFF). The Pritzker Prize has been awarded annually since 2011 by MJFF to recognize researchers who make an exceptional contribution to Parkinson’s research and exhibit a commitment to mentoring the next generation of Parkinson’s scientists. Dr. Lee is the first female researcher to be selected for the Pritzker Prize. She was presented the prize at a Foundation event in New York City in November.
Virginia Lee, the John H. Ware 3rd Endowed Professor in Alzheimer’s Research at the Perelman School of Medicine at The University of Pennsylania, received the 2018 Robert A. Pritzker Prize for Leadership in Parkinson’s Research from the Michael J. Fox Foundation for Parkinson’s Research (MJFF). The Pritzker Prize has been awarded annually since 2011 by MJFF to recognize researchers who make an exceptional contribution to Parkinson’s research and exhibit a commitment to mentoring the next generation of Parkinson’s scientists. Dr. Lee is the first female researcher to be selected for the Pritzker Prize. She was presented the prize at a Foundation event in New York City in November. The University of Pennsylvania has named Zeid Ra’ad Al Hussein, the United Nations High Commissioner for Human Rights (2014-2018), the Distinguished Global Leader-in-Residence at Perry World House (PWH) for spring 2019. In addition to his residency at PWH, Penn’s global policy research institute, Dr. Al Hussein will also co-teach a class at the Penn Law School during the spring semester.
The University of Pennsylvania has named Zeid Ra’ad Al Hussein, the United Nations High Commissioner for Human Rights (2014-2018), the Distinguished Global Leader-in-Residence at Perry World House (PWH) for spring 2019. In addition to his residency at PWH, Penn’s global policy research institute, Dr. Al Hussein will also co-teach a class at the Penn Law School during the spring semester. Murray Griffin Murphey, emeritus professor of history in the School of Arts and Sciences at the University of Pennsylvania, died December 6. He was 90.
Murray Griffin Murphey, emeritus professor of history in the School of Arts and Sciences at the University of Pennsylvania, died December 6. He was 90. Firooz Aflatouni, the Skirkanich Assistant Professor of Electrical and Systems Engineering in Penn’s School of Engineering and Applied Science, has been awarded a NASA Early Stage Innovations grant to design and implement arrays of optical antennas that can enable laser communication in near-Earth satellites, which will be more efficient and carry far more information than microwaves.
Firooz Aflatouni, the Skirkanich Assistant Professor of Electrical and Systems Engineering in Penn’s School of Engineering and Applied Science, has been awarded a NASA Early Stage Innovations grant to design and implement arrays of optical antennas that can enable laser communication in near-Earth satellites, which will be more efficient and carry far more information than microwaves. Dan Dongeun Huh, Wilf Family Term Assistant Professor in the department of bioengineering in Penn’s School of Engineering and Applied Science, and his BIOlines research group were recently recognized with the Science Award in the 2018 Lush Prize for work on microfabricated devices that mimic the function of various organs using living cells.
Dan Dongeun Huh, Wilf Family Term Assistant Professor in the department of bioengineering in Penn’s School of Engineering and Applied Science, and his BIOlines research group were recently recognized with the Science Award in the 2018 Lush Prize for work on microfabricated devices that mimic the function of various organs using living cells. Penn Dental Medicine periodontics resident Kang Ko (D’15, GD’20) was selected by the American Academy of Periodontology (AAP) Foundation as a 2018 recipient of the AAP Educator Scholarship. The selection committee presented the award during the AAP Annual Meeting, held October 27-30 in Vancouver, British Columbia.
Penn Dental Medicine periodontics resident Kang Ko (D’15, GD’20) was selected by the American Academy of Periodontology (AAP) Foundation as a 2018 recipient of the AAP Educator Scholarship. The selection committee presented the award during the AAP Annual Meeting, held October 27-30 in Vancouver, British Columbia. A grant awarded to Penn Dental Medicine and the Children’s Hospital of Philadelphia will help create a new program that focuses on providing dental care to children and adults with a rare genetic disorder, Cornelia de Lange Syndrome (CdLS). Since many children with CdLS have cognitive issues, dental care is often performed under sedation and requires experienced pediatric specialists to deliver proper dental care.
A grant awarded to Penn Dental Medicine and the Children’s Hospital of Philadelphia will help create a new program that focuses on providing dental care to children and adults with a rare genetic disorder, Cornelia de Lange Syndrome (CdLS). Since many children with CdLS have cognitive issues, dental care is often performed under sedation and requires experienced pediatric specialists to deliver proper dental care.











