Over ten years ago I came to the University Library System with more than 15 years of library experience. What attracted me was the benefit package. I had worked previously in Drexel University's Library and then in a Federal Government library. My plan here at Penn was to finish my own education and provide an excellent education for my family.
It was with great interest that I read articles about our new University President when she first arrived. She spoke often about (I believe the term was) "University excellence." We were to strive for excellence here at Penn. I believe I have kept my part of the bargain, but I feel the administration hasn't kept theirs.
Isn't our "business" education? Then why would we even suggest cutting into any type of educational benefit? Shouldn't we be trying to get more of our employees and their families to get degrees?
Aren't we striving for excellence? Then why are we looking to businesses in the area and following their example? Shouldn't we be setting the example?
I was told at the benefits meeting held here at the law school that money had to be saved somewhere; if not on benefits, where? I don't know, but I do know that you do not attract and keep excellent people by taking away things they were promised when they came, even if it is just being let off early a half hour a day during the summer.
My challenge to the Administration is to keep the excellence we have and to set an example of excellence for others--in education, in benefits, and in the morale of its employees.
-- Joseph F. Parsio, Assistant Head of Stacks,
Biddle Law Library, Circulation Department
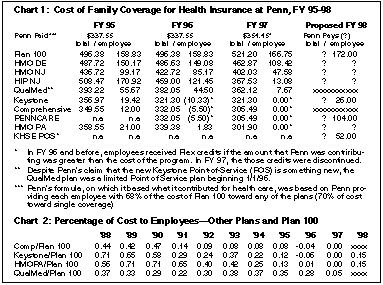
Dr. David Hackney's description of the decision to aggressively price the PENNCare option confirmed what many people had suspected: that Penn and its Health Systems subsidiary had conspired to use predatory pricing to create the conditions under which a popular low cost health insurance option could be eliminated and replaced with a high-priced option that would funnel our hard earned dollars into a wholly owned subsidiary of University of Pennsylvania, Inc. It was a variation on the classic bait and switch practices that have been outlawed for most retail products. How predatory the pricing was can be seen in charts 1 and 2.
Chart 1 shows how, for the last two years, Health Systems has priced PENNCare at the same rate as the least or second least expensive health care option--Blue Cross Comprehensive--in order to attract business from other providers. The Comprehensive Plan was particularly targeted--PENNCare offered everything Comprehensive did and much more, for the exact same price. Chart 2 demonstrates how the Comprehensive plan has always been among the most affordable options; and has averaged well under 10% of the cost of Plan 100 coverage since 1991. PENNCare will cost 60% of the price of Plan 100.
The Comprehensive Plan was specifically designed to provide employees with a low-cost alternative to traditional indemnity plans. It was a plan designed to be competitive with HMOs, and in fact was considerably cheaper than the HMOs for most of the last ten years. Because of the ridiculously low pricing of PENNCare for the last two years, 25% of employees changed to the UPHS plan. Now that PENNCare has a large chunk of the market, the affordable option that the Comprehensive Plan offers is being eliminated--supposedly because of low enrollment. But it is obviously that the cause of the low enrollment was the predatory pricing of PENNCare. Penn Care is going up in cost to employees by $109.50; the most expensive plan is going up in cost by less than $14.
Not only are these kind of tactics immoral, they also cost employees time and money, and pose a potential risk to the health of Penn's workers and their families. People have changed their family doctors to participate in PENNCare; they have chosen pediatrician for their children. They have chosen new cardiologists for treatment of their heart disease. Now, they will either have to change back, or pay an unconscionable increase in their health care premiums. And every time you change doctors, you put yourself at risk because you lose the security that continuity of service provides.
The Rodin/Fry administrators were well aware that Health Systems was deliberately engaged in unethical practices designed to eliminate the competition, yet did nothing to protect the interests of employees. There is something extremely wrong when University administrators will permit their employees to be placed at risk for the benefit of one of its subsidiary corporations.
It is clear what is happening here--UPHS and Penn conspired to engage in predatory pricing to grab a large share of the market and eliminate much of the competition--and then raise prices to employees. It is equally clear that the primary concern of the Benefits Redesign Committee --dominated as it was by upper level administrators and UPHS affiliated medical professionals--was not maintaining affordable health care options for Penn employees, but maintaining a robust and healthy profit margin to justify the bloated salaries UPHS administrators. Over the last couple of years, Judith Rodin, John Fry, and William Kelley have assumed extraordinary risks on behalf of Penn and UPHS in order to expand Health Systems. We, Penn's faculty and staff, are now being told to pay the cost of assuming that risk.
This entire Benefits Redesign Plan needs to be completely junked, and a committee of faculty and support staff needs to start the process over. Penn's administrators have demonstrated that their priorities and ethics are incompatible and inconsistent with the academic mission of this University, and the legitimate interests of the people who work at Penn.
-- Paul Lukasiak,
Administrative Assistant, SSW

Mr. Lukasiak believes that the change in the pricing of PENNCare represents, and that the entire health care redesign represents, predatory pricing. He bases this claim on the initial low price of PENNCare, which he believes was to eliminate competition, followed by the recommended price increase in the Benefits Redesign proposal, which he believes was to secure an unfair return to UPHS or the University. This claim is entirely without merit. In predatory pricing, the goal is to eliminate competition. Under the recommended Benefits Redesign, competition is actually increased and not decreased. This is the opposite of Mr. Lukasiak's claims. With the new point-of-service plan (POS), competition among all providers increases and, in fact, the Keystone POS option, with its larger network of primary care providers, is in an advantaged position relative to UPHS.
When PENNCare was first offered, neither the University nor UPHS knew at what level to set premium rates because enrollment and actual claim experience could not be predicted in advance. It was decided to set the PENNCare price, provisionally, at the same level as the Comprehensive plan until actual claim experience was determined. The fact that that price was zero, reflects the malfunctioning of the health care pricing formula, a malfunctioning which we have elaborated on throughout our communications in recent weeks. All plan options, except Plan 100, were priced at zero, including plan options offered by providers other than UPHS. Mr. Lukasiak's own tables, Charts 1 and 2, reflect that malfunctioning. At a time when medical costs and cost-sharing were increasing, Penn's employee contributions were declining. The recommendations reestablish cost-sharing based on the percentage sharing from 1994. None of these factors suggest predatory policy; instead they reflect the opposite: increased choice among competing providers with relative price differences reflecting difference in plan costs, and with cost-sharing equal to that of just three years ago.
The decision to price PENNCare at the level of Comprehensive left both priced inappropriately. If employees left the Comprehensive plan for PENNCare, it clearly was not because of the pricing of PENNCare as is suggested in the letter. Moreover, while some employees in the Comprehensive plan did move to PENNCare (the majority did not), the low enrollment in the Comprehensive plan pre-dated the introduction of PENNCare and is not the result of the introduction of that program as claimed.
Now that we have actual claim experience, we know that the contributions for the PENNCare option were set too low, that it was not a cost-efficient plan, and that an increase in contributions is indicated. The factors that make the PENNCare plan attractive to employees--rich benefits, no contributions and lack of restrictions on access to care--also make the plan too expensive for Penn to provide without changes in cost-sharing.
Our comments in Almanac on the similarity of the out-of-network benefits in the point-of-service and the benefits in the Comprehensive plan were in response to questions about the plans. While there are differences in the two plans that our employees will need to evaluate at Open Enrollment, the point-of-service plan may offer an acceptable and more affordable option to employees in the Comprehensive plan than accessing the benefit under PENNCare. It is the case that individuals in the Comprehensive plan will face some cost sharing as they move to other options in the new plan, as is the case with all other employees. It is also the case that the costs and the cost-sharing in all plans will be greater than in the HMOs. The committee has been very open with the community about the lower cost-sharing in the HMOs because the majority of Penn's lower-paid employees are in those plans. This is a principle set early on by the Benefits Redesign Committee and one that we hope will continue to guide decisions about health benefits costs.
-- Barbara Lowery, Associate Provost
-- H. Clint Davidson, Vice President/HR
Co-chairs, Benefits Advisory Committee
____________________
Speaking Out welcomes reader contributions. Short timely letters on University issues can be accepted Thursday noon for the following Tuesday's issue, subject to right-of-reply guidelines. Advance notice of intention to submit is appreciated.--Ed. �
Almanac
Volume 43 Number 26
March 18, 1997
Return to Almanac's homepage.
Return to index for this issue.